Recent Posts
- Loic Fort leaving for faculty position!
- (no title)
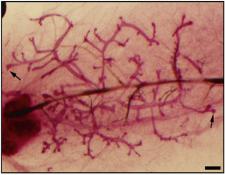
- Mammary Organoid
- Alex gets the cover of Developmental Cell, July 2023!
- Our Research Group
Recent Comments
Archives
Categories
Meta
EPITHELIAL CELL BIOLOGY
The Macara laboratory is fascinated by epithelia, which were the first tissue type to evolve with the rise of multicellular animals, and which form all of the organs that contact the external world – skin, intestine, exocrine glands, lungs, kidneys, etc.
Remarkably, embryonic stem cells and pluripotent stem cells (ESCs and iPSCs) are epithelial. In many organs, epithelia are maintained by adult stem cells.
Strikingly, over 90% of human cancers arise from epithelia.
Epithelial cells are characterized by apical-basal polarity, and by intercellular junctions.
Epithelial cells exhibit collective decision making. They talk to each other to decide whether to divide, or migrate, or extrude from the tissue.
We are interested in how epithelia maintain homeostasis and how this is lost in cancer; how epithelial stem cells respond to damage; how cell lineage is maintained and altered; and how epithelia achieve and maintain cell polarization. We are also very interested in why ESCs and iPSCs are epithelial, and how these cells lose their epithelial nature when they turn into mesoderm and cardiomyocytes. We use multiple mouse models, in vivo fluorescence imaging, CRISPR screens ,single molecule imaging, and organoid cultures to investigate these problems.
CELL POLARITY AND APICAL PROTEIN DELIVERY
The Crumbs polarity proteins are apical transmembrane proteins that maintain cell polarity and interact with the Hippo pathway to control cell proliferation. How Crumbs reaches the apical surface, and how/when it interacts with other components of the polarity machinery, remains a mystery. A grad student in the lab, Christian de Caestecker, has discovered a fundamentally important new way in which apical membrane proteins are separated from other membrane proteins to ensure their correct delivery. His work is now published online at Nature Cell Biology (2024). He developed knock-in CRISPR cell lines in which Crumbs is tagged with a fluorophore so we can detect single molecules in living cells. He has also created a so-called RUSH system in which Crumbs is trapped and accumulates in the endoplasmic reticulum until it is released by the addition of biotin. It then transits synchronously through the Golgi to the apical plasma membrane. The ability to track molecules at each step of this process has led to new insights into the polarized traffic of this key protein to the apical cell cortex. With Savi Buluwana, an undergrad honors student, he has developed a genome-wide CRISPR KO screen to identify genes that are essential for correct apical delivery of Crumbs.
EMBRYONIC STEM CELLS, EMT AND APOPTOSIS
Human iPS cells and ES cells are epithelial, with robust apical/basal polarity. Interestingly, this epithelial character is essential for pluripotency. Loic Fort, a postdoc in the lab, discovered that widespread apoptosis occurs shortly after activating the WNT pathway, which is the first step towards mesoderm lineage specification. Through a series of clever experiments, Loic found that “find-me” signals released by the apoptosing cells, are essential to permit their surviving neighbors to respond to WNT and begin the transition towards mesoderm (Nature Cell Biol 2022). This is a completely novel function for these signals, which normally attract macrophages to engulf the dying cells.
CELL INTERCALATION, CELL EXTRUSION, AND CANCER
A common idea, widely discussed in the literature, is that an early event in the initiation of cancers is loss of oriented mitosis. Alex Pfannenstein investigated this idea by generating CRISPR-edited cell lines in which the spindle orientation mechanism is defective. Remarkably, he found that rather than creating multiple layers, the daughter cells in these lines re-integrate back into the epithelial layer to maintain their normal organization. Alex also developed a new assay to observe re-integration of cells into the epithelium and used it, together with intraductal injections of cells into mice, to investigate the molecular mechanisms involved in this fascinating behavior (Dev Cell, 2023). He is now a postdoc with Tobias Meyer at Cornell.
Aishwarya Venkataravi, a new postdoc, and Miki Daniel, our lab manager, are following up on this work to understand the fundamental mechanisms of cell re-integration, and the process by which tumor cells escape the mammary ducts into the surrounding stroma.
Paola Molina, a postdoc in the lab, is investigating the mechanisms by which cancer cells get extruded from epithelial monolayers, using CRISPR screens, live cell imaging and other approaches.
 EPITHELIAL STEM CELLS AND THEIR RESPONSE TO DAMAGE
EPITHELIAL STEM CELLS AND THEIR RESPONSE TO DAMAGE
A fundamental biological question is how epithelia maintain integrity in the face of continual stresses and damage. Lindsey Seldin, (now on the faculty at Emory University) asked how the skin and mammary gland respond to DNA damage. She discovered a remarkable series of events occurs when these tissues, in the mouse, are exposed to DNA cross-linking agents. The basal cells (which form the epidermal stem cells in skin) rapidly proliferate and their progeny undergo lineage mis-specification. Lindsey discovered that these effects are non-cell autonomous, which means they are indirectly caused by other cells in the tissue. She found that dermal fibroblasts respond to DNA damage by activating a part of the innate immune system called the NLRP3 inflammasome. This triggers release of the cytokine IL1-beta, which turns on cell proliferation and lineage mis-specification in the basal stem cells. This work was published in Developmental Cell (2020), was highlighted on the cover, and was discussed in an accomanying Preview article.l
PROTEIN COMPLEX DYNAMICS – SINGLE MOLECULE IMAGING
Mukhtar, a former postdoc in the laboratory, discovered a few years ago that the PAR3 polarity protein functions at epithelial tight junctions as a receptor for the Exocyst, an octameric complex that tethers vesicles at the plasma membrane to promote fusion (Nat Commun 2017). Exocyst is essential for the delivery of membrane proteins and secreted proteins. With another postdoc, Hisayo Nishida-Fukuda, they used CRISPR/Cas9 editing to create epithelial cells that express fluorophore-tagged alleles of multiple exocyst subunits. Coupled with high speed, ultrasensitive TIRF and near-TIRF multi-channel microscopy, single exocyst molecules can be detected, and their movements tracked in real time within living cells (Nat Commun 2018).
In collaboration with geneticists in Australia, we demonstrated vesicle fusion defects in cells from a human patient with a mutation in one of the exocyst subunits (J Exp Med 2020). This mutation provides a powerful tool for further analysis of exocyst mechanism.